Client: HealthPartners
Project: "Ease of Use" Claims & Balances
Role: User Experience Designer
Business Goal: Visually update the design and align desktop and mobile experiences; Illustrate the value of the insurance plan; Improve the user experience by making claims, deductibles, and coverage easier to understand.
Audience: HealthPartners members and member-patients
User Goals: Make it easy to see when my claim is ready to view; make it easy to understand what portion of the claim was covered by my insurance plan; make it easy to understand what portion of the claim I am responsible for.
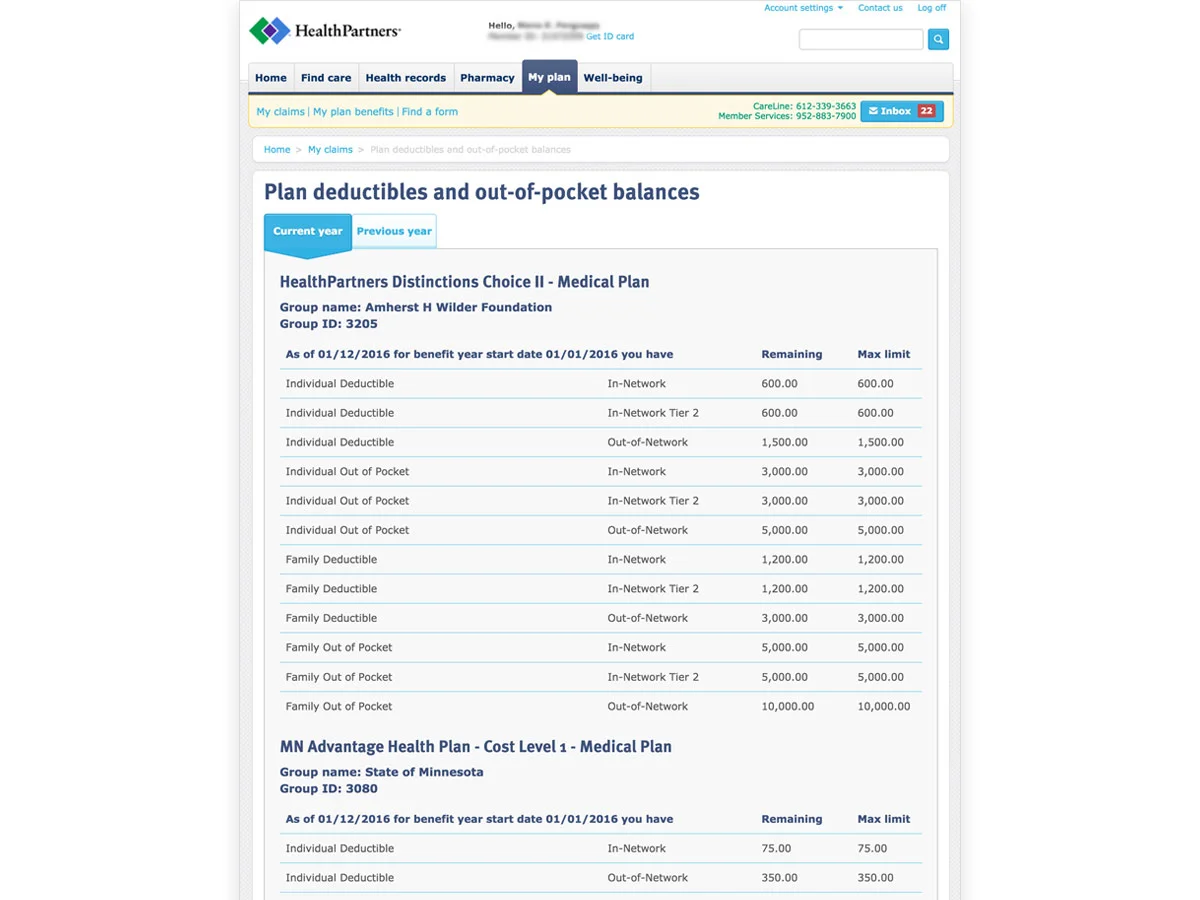
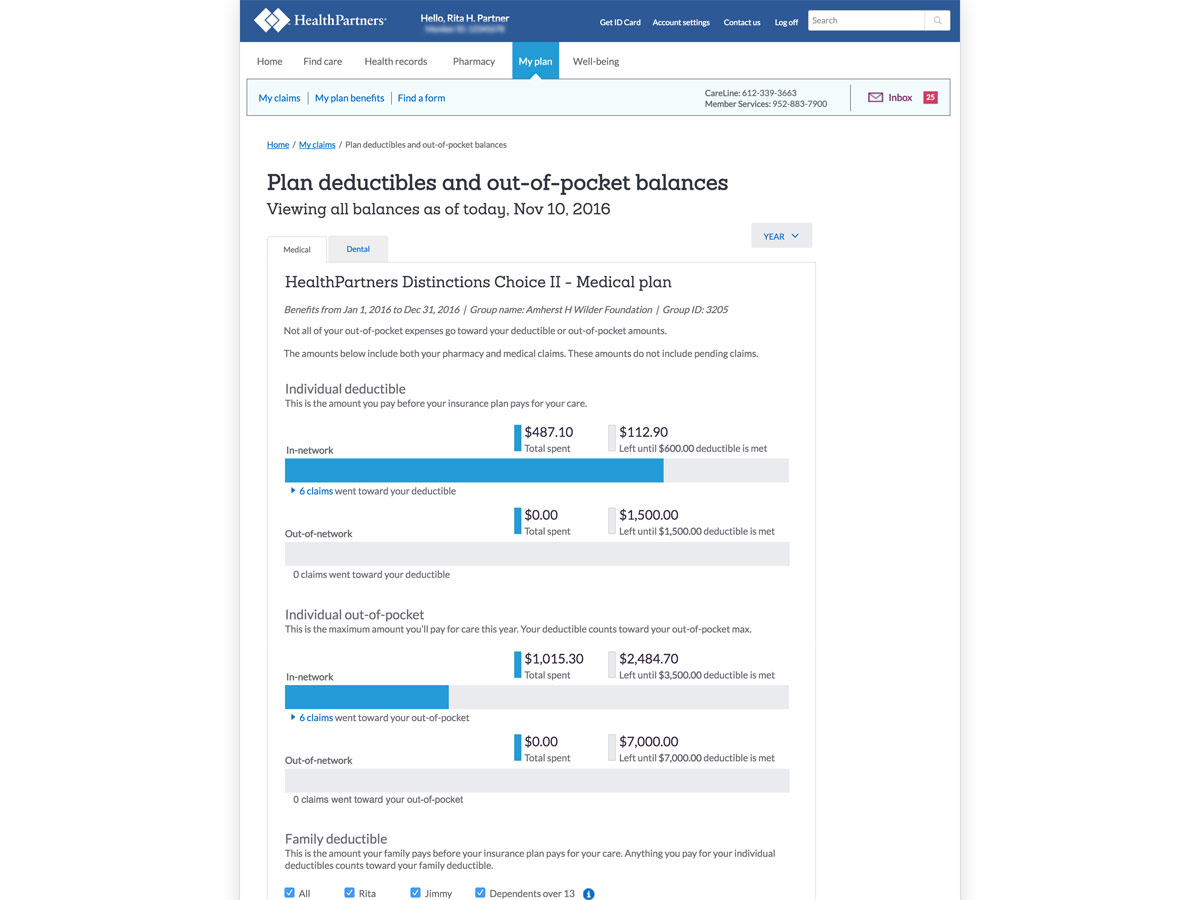
Description: The new My Plan and Claims experience greatly streamlines the claims experience for users by making it easier to understand when a claim is ready to view, how much was covered by insurance, and how much you owe.
After initial prototyping, we tested our design solutions with users. We employed Leede Research for 6 usability testing sessions. We had 6 users covering a range of age and familiarity with health care, come in and conduct tasks using our designed screens.
· Plan information - Can they find benefit/coverage details; Can they see where their dependents are listed
· Claims information - What is the most important data value to identify a claim (Date, Member, Provider, Description, Claim type, Total billed, Amount I owe); Do they notice the status indicators (denied icon)
· Spending & Savings information - Can you find your status of your deductible and Oop max; Can you find the status of your accounts
The results of the test uncovered that the design of the pages were satisfactory for users - everyone was able to find the information we asked them to find. However, understandability of the complex concepts, (what is a deductible, what is a negotiated discount, what is an HSA) failed across most users. The conclusion was that the interface design was approved for development, but integrating a "guided experience" to help educate users on confusing topics was a recommendation for future iterations.
• EXPERIENCE DESIGN •